Bunions
Even though bunions are a common foot deformity, there are misconceptions about them. Many people may unnecessarily suffer the pain of bunions for years before seeking treatment.
What Is a Bunion?
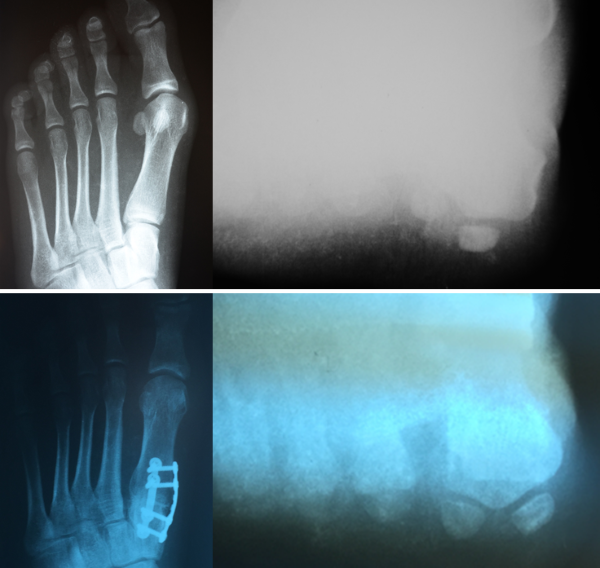
A bunion (also referred to as hallux valgus) is often described as a bump on the side of the big toe. But a bunion is more than that. The visible bump actually reflects changes in the bony framework of the front part of the foot. The big toe leans toward the second toe, rather than pointing straight ahead. This throws the bones out of alignment—producing the bunion’s bump.
Bunions are a progressive disorder. They begin with a leaning of the big toe, gradually changing the angle of the bones over the years and slowly producing the characteristic bump, which becomes increasingly prominent. Symptoms usually appear at later stages, although some people never have symptoms.
Causes
Bunions are most often caused by an inherited faulty mechanical structure of the foot. It is not the bunion itself that is inherited but certain foot types that make a person prone to developing a bunion.
Although wearing shoes that crowd the toes will not actually cause bunions, it sometimes makes the deformity get progressively worse. Symptoms may therefore appear sooner.
Symptoms
Symptoms, which occur at the site of the bunion, may include:
- Pain or soreness
- Inflammation and redness
- A burning sensation
- Possible numbness
Symptoms occur most often when wearing shoes that crowd the toes, such as shoes with a tight toe box or high heels. This may explain why women are more likely to have symptoms than men. In addition, spending long periods of time on your feet can aggravate the symptoms of bunions.
Diagnosis
Bunions are readily apparent—the prominence is visible at the base of the big toe or side of the foot. However, to fully evaluate the condition, the foot and ankle surgeon may take x-rays to determine the degree of the deformity and assess the changes that have occurred.
Because bunions are progressive, they do not go away and will usually get worse over time. But not all cases are alike—some bunions progress more rapidly than others. Once your surgeon has evaluated your bunion, a treatment plan can be developed that is suited to your needs.
Nonsurgical Treatment
Sometimes observation of the bunion is all that is needed. To reduce the chance of damage to the joint, periodic evaluation and x-rays by your surgeon are advised.
In many other cases, however, some type of treatment is needed. Early treatments are aimed at easing the pain of bunions, but they will not reverse the deformity itself. These include:
- Changes in shoewear. Wearing the right kind of shoes is very important. Choose shoes that have a wide toe box and forgo those with pointed toes or high heels, which may aggravate the condition.
- Padding. Pads placed over the area of the bunion can help minimize pain. These can be obtained from your surgeon or purchased at a drug store.
- Activity modifications. Avoid activity that causes bunion pain, including standing for long periods of time.
- Medications. Oral non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be recommended to reduce pain and inflammation.
- Icing. Applying an ice pack several times a day helps reduce inflammation and pain.
- Injection therapy. Although rarely used in bunion treatment, injections of corticosteroids may be useful in treating the inflamed bursa (fluid-filled sac located around a joint) sometimes seen with bunions.
- Orthotic devices. In some cases, custom orthotic devices may be provided by the foot and ankle surgeon.
When Is Surgery Needed?
If nonsurgical treatments fail to relieve bunion pain and when the pain of a bunion interferes with daily activities, it is time to discuss surgical options with a foot and ankle surgeon. Together you can decide if surgery is best for you.
A variety of surgical procedures is available to treat bunions. The procedures are designed to remove the bump of bone, correct the changes in the bony structure of the foot and correct soft tissue changes that may also have occurred. The goal of surgery is the reduction of pain and deformity.
In selecting the procedure or combination of procedures for your particular case, the foot and ankle surgeon will take into consideration the extent of your deformity based on the x-ray findings, your age, your activity level and other factors. The length of the recovery period will vary, depending on the procedure or procedures performed.


Learn About Lapiplasty® Treace Medical Concepts
Have you heard the buzz about Lapiplasty®? It’s time to learn what all the fuss is about.
This revolutionary surgery is newly available here at the Foot and Ankle Center of the Rockies and is being hailed as a breakthrough for bunion surgery. Dr. Daniel J. Hatch worked together with Treace to develop this cutting-edge procedure and is now excited to be able to offer it to people struggling with bunions in Northern Colorado.
For 87% of people with bunions, traditional bunion surgery fails to get to the true source of the problem. This leaves many patients still in pain and unhappy with both the look and function of their foot after surgery. But don’t worry — there’s a better way to completely solve your bunions. Lapiplasty® is a three-dimensional bunion correction surgery that gets to the root of the problem to fully, permanently correct the deformity.
If you want to learn more about this exciting new surgical treatment, check out these in-depth educational resources.
Bunion Surgery Video
Visual learners will enjoy this animated, three-dimensional look at how the bunion deformity happens, and how Lapiplasty® effectively corrects the problem at the source.
Contrary to popular belief, bunions are often complex deformities that stem from joint issues deep in the foot. Most bunion treatments, like osteotomies, only address the top part of the metatarsal, leaving the root of the problem — the unstable joint — untouched. This video gives you a 3D look at how Lapiplasty® can precisely realign the entire metatarsal bone, correcting the unstable joint to permanently solve the bunion problem.
Dr Hatch talks about Lapiplasty®
Before and After Surgery

Left foot pre operative

Left foot post operative
Read the Brochure
One in three patients are unhappy with the result of their traditional bunion surgery — don’t be one of them! This brochure includes testimonials from real Lapiplasty® patients, so you can hear about the benefits from people who have actually experienced them. Have your questions answered with the frequently asked questions section, and learn with clear X-rays and diagrams why traditional bunion surgeries can’t measure up to Lapiplasty®.
Log in to the “Patients” Page
Looking for more in-depth information on Lapiplasty®, or ready to find a surgeon in your area? The Lapiplasty® patient page has everything you need to make an informed decision and reach out to a surgeon to move forward with correcting your bunion.
The patient page is your hub for information about Lapiplasty®. Featuring everything from an interview with a podiatrist about the procedures to statistics about both Lapiplasty® and traditional bunion surgeries, to real patient’s stories about their own surgeries, you can have your questions answered and make sure you have a complete understanding of the procedure to facilitate your health decisions.
This page even features a search function to help you find a Lapiplasty® surgeon near you. This easy-to-use locator requires only your zip code or city to find the closest and most convenient surgeon. Your search results include each surgeon’s phone number, so you can quickly and easily call to schedule a consultation and see if Lapiplasty® is right for you. If you’re in the Northern Colorado area, Dr. Daniel J. Hatch helped develop this procedure and is happy to consult with you about your eligibility.
Don’t let bunions keep you from your active, normal lifestyle. Lapiplasty® is the new frontier in bunion surgery, and can finally put an end to the pain, discomfort, and limitations that bunions have caused you to suffer. Best of all, you’ll be back on your feet just a few weeks after surgery! Talk to your doctor today about how Lapiplasty® can get to the root of your bunion deformity.